Ditching Dairy Can Alleviate Arthritis Pain is a guest post by Rick Scott (#veganhockeyplayer)
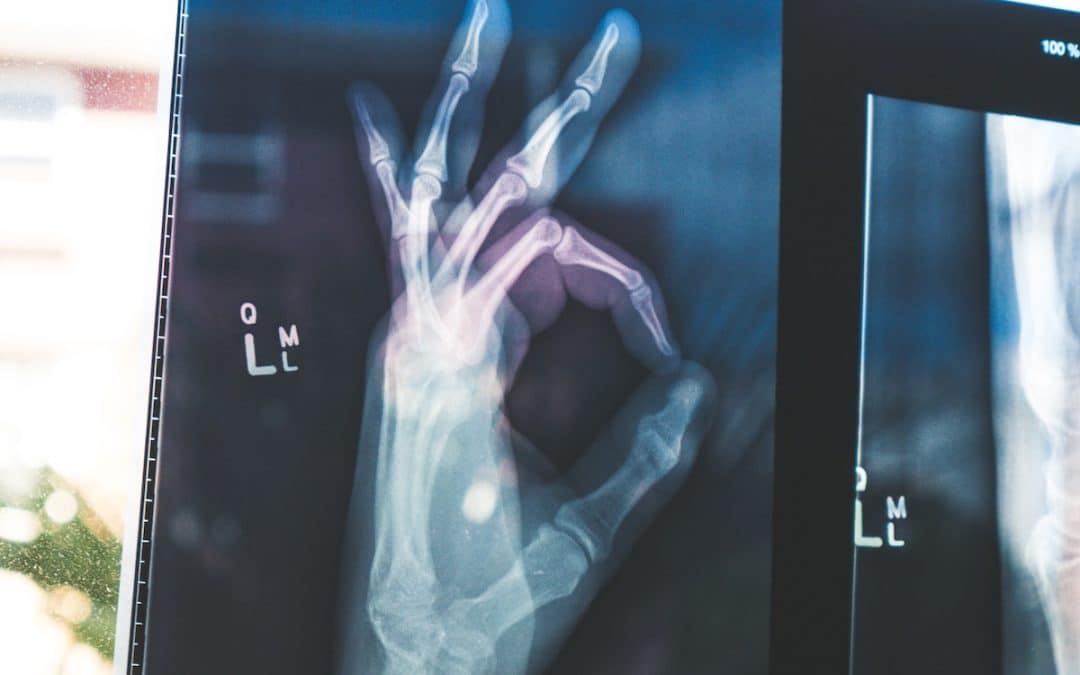
The first time that I broke my wrist was in a 1983 on-ice collision when I was an 18-year-old hockey player. I broke my thumb near the same wrist a couple of years later in a bike race. When I broke the wrist again in 2007 in another bike race, the orthopedic doctor looked at the x-ray and exclaimed, “Look at all that arthritis!”
Rick’s story
As a veteran athlete, I assumed that you forever feel the aches and pains of a lifetime of injuries as we age, typically in the form of arthritis when it comes to broken bones and joint injuries. I taped my right wrist in the gym for years and wore a brace on it when I went back to playing hockey shortly before my fiftieth birthday. I lived with the soreness daily and I certainly never expected the miracle healing that occurred when I removed dairy from my diet.
I went vegetarian 25 years prior to going vegan, which I did five years ago, coinciding with my transition back from bike racer to hockey player. On the ice, hockey players rely on their wrists for shooting, stick handling, and passing so I depended upon the brace my doctor gave me after the second break. When I removed dairy from my diet, I started noticing the soreness that I felt in my wrist for several decades had diminished. It felt so good that I stopped wearing the brace. To my surprise, the discomfort that I had lived with in my wrist since the mid-1980s disappeared completely and the only thing that changed is that I stopped consuming dairy products.
The physician’s perspective
During a recent podcast interview, I shared my story with listeners, and it made me curious about how dairy impacts arthritis. Is what I experienced normal or a rare exception? I reached out to Dr. Micah Yu, a rheumatologist, board-certified internal medicine doctor, and a certified lifestyle medicine doctor who practices at The Institute of Plant-Based Medicine in Newport Beach, California, to get the science behind my remission. Dr. Yu has autoimmune arthritis, but with a whole-foods, plant-based diet, he was able to significantly improve his condition without medication. The form of arthritis that impacted me was osteoarthritis.
“Osteoarthritis is a wear-and-tear arthritis that can be seen in the elderly, athletes, and people from the military as well from all the trauma they sustain. What we are finding out is that in osteoarthritis, even though it is not an autoimmune arthritis, there is an inflammatory component that we are discovering now at the bone,” said Dr. Yu.
“When you eat a whole-foods, plant-based diet, you are avoiding inflammatory foods such as dairy, processed food, refined sugar, and red meat, which can be inflammatory. Patients find meat to be inflammatory as shown by arthritis symptoms versus a patient that goes on a whole-foods, plant-based diet. Certain types of oil can be very inflammatory as well, especially if you cook it above the boiling point. Everyone is different, but a whole- foods, plant-based diet can be very therapeutic for people when they have arthritis.”
Managing inflammation
With the coronavirus threat, we have become keenly aware of the need to maintain a strong immune system. Another reason to bolster the immune system is that it plays a role in fighting inflammation.
“Where the immune system is connected is that 60-70 percent of the immune system is in the gut. In order to help the immune system send anti-inflammatory signals, one of the key steps is fiber. Fiber is anti-inflammatory. That, along with short-chain fatty acids, sends out anti-inflammatory signals in the gut, which then travel to the rest of the body through the bloodstream and the lymphatic system. That is why a whole-foods, plant-based diet is so therapeutic,” explained Dr. Yu.
He continued, “A high-fat diet is inflammatory. It can induce inflammatory signals in the area of the gut and send inflammatory signals throughout the rest of the body.”
Let’s be clear: not everyone will be cured from osteoarthritis like I was just by ditching dairy and adopting a whole-foods, plant-based diet, but it is common to experience varying degrees of relief. It is important to consider that arthritis is impacted by factors beyond food, according to Dr. Yu.
“Lifestyle factors also play a role such as stress levels. How much does someone exercise? How much do they sleep? Do they smoke? Do they do drugs? And how is their emotional well-being? How much radiographic damage is there on the x-rays? There is an inflammatory component to osteoarthritis. If you cut out most of the inflammatory foods such as processed food, refined sugar, and dairy, then you can give yourself a head start in improving your symptoms of osteoarthritis. The x-ray findings are not going to get better, meaning the damage of joints is not going to get better, but if you calm down the inflammation, then you can possibly have less pain in the area.”
Omega-3s and inflammation
Eager to further explore and understand the connection between inflammatory foods and arthritis, I hit the internet where I came across this passage in regards to omega-3 fatty acids and athletics that concludes “A plant-based diet, free of dairy foods, is high in omega-3 fatty acids, which help reduce inflammation and swelling, and low in omega-6 to help produce the optimal 2:1 ratio of omega-6 to omega-3.” (1)
Dr. Yu said, “I always recommend that my patients eat fruits, vegetables, legumes, whole grains, lentils, beans, quinoa, and flaxseeds for omega-3 fatty acids. With fruits and vegetables, you want to focus on the fiber. It’s like the most important nutrient out there for inflammation. The phytonutrients in the fruit and vegetables are very healing and anti-inflammatory. Spices can be very beneficial as well: turmeric, ginger, and green tea.”
Antioxidants and inflammation
Athletes tend to be vigilant about reducing inflammation from the stress and strain of athletic activity because of its adverse effect on athletic performance. However, athletes and nonathletes alike benefit from reducing inflammation caused by food. What should we be eating to fight inflammation? Foods rich in antioxidants. That means spices as mentioned in the preceding paragraph; dark leafy greens like kale, spinach, and collards; select fruit such as strawberries, blueberries, raspberries, oranges, and cherries; nuts; tomatoes; and beans.
Dr. Yu urges patience when it comes to using “food as thy medicine and medicine as thy food.” Even in my case, arthritis did not disappear overnight. It was over time that I noticed the benefits of my dairy-free, plant-based diet.
“You’re not going to see any impact if you consume turmeric, ginger, or green tea once a week. With food, you’ve got to think long-term gains. It’s not like medicine where you take a pill and an hour later the pain is gone. That’s not the way food works. It’s a long process, a day-to-day consistency of habits formed over a long period of time that can be very beneficial.”
Learn how you can take your first steps towards ditching dairy.
References
- Simopoulos AP. Curr Sports Med Rep. 2007 Jul; 6(4):230-6